H. Pylori: Symptoms, Causes, Test & Treatment Guide

The human stomach is a marvel of biological engineering, a highly acidic environment designed to break down food and neutralize most invading pathogens. Yet, there is one specific, spiral-shaped bacterium that has evolved to thrive in this harsh landscape: Helicobacter pylori, or H. pylori.
For many people, the realization that they have a bacterial infection in the stomach comes as a surprise. It’s often discovered during a routine check-up or after weeks of persistent, nagging discomfort that just won’t go away with over-the-counter antacids.
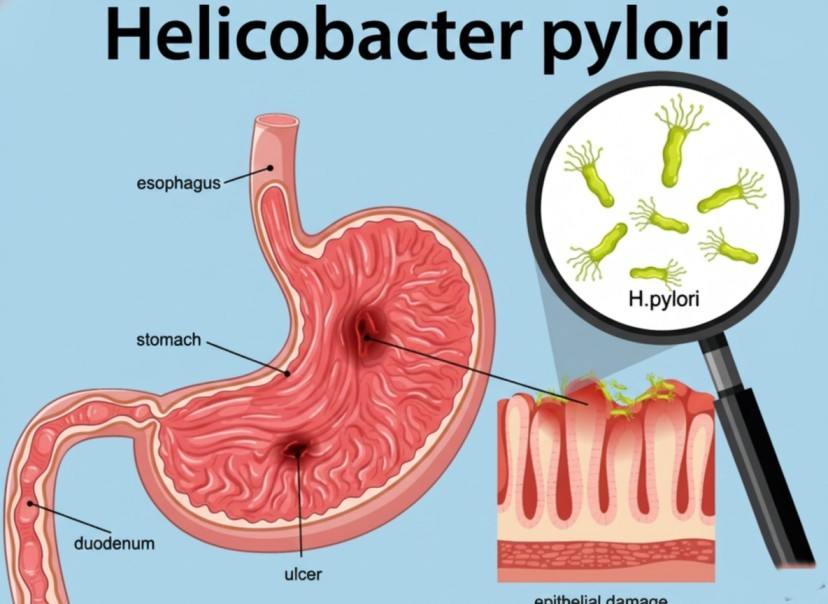
Understanding what is H. pylori is the first step toward regaining digestive health. It isn’t just a simple “stomach bug”; it is a sophisticated organism that, if left unaddressed, can lead to chronic gastritis and peptic ulcer disease.
In his clinical practice, Dr. Samir Rahmani often sees patients who have spent months trying to self-diagnose vague symptoms like bloating or a dull ache in the upper abdomen. The journey to healing begins with an accurate H. pylori test and a structured, medically supervised treatment plan.
What is H. pylori Infection?
Helicobacter pylori is a type of bacteria that infects the stomach lining. It is remarkably common—estimates suggest that nearly half of the world’s population carries it, though not everyone becomes symptomatic. The bacteria are uniquely adapted to survive the stomach’s acidity by producing an enzyme called urease, which neutralizes gastric acid in its immediate vicinity.
When we discuss what is H. pylori infection, we are really talking about the way these bacteria burrow into the protective mucosal lining of the stomach. By doing so, they weaken the barrier that protects the stomach wall from its own acid. This often results in gastritis, which is a formal term for the inflammation of the stomach lining. Over time, this inflammation can erode the tissue, leading to the development of a stomach ulcer.
The Origins: H. Pylori Causes
How does one actually contract a stomach bacterial infection? While the exact transmission route is sometimes debated, it is generally believed to spread through:
Person-to-person contact: Saliva, vomit, or fecal matter are primary vectors.
Contaminated sources: Tainted water or improperly cleaned food.
Environmental factors: Living in crowded conditions or areas without a reliable clean water supply increases the risk.
Most people actually acquire the infection during childhood, though they may not develop H. pylori symptoms until much later in adulthood when the chronic inflammation finally reaches a tipping point.
Recognizing H. Pylori Symptoms: The Body’s Warning Signs
The tricky part about H. pylori is that it can be a “silent” resident for years. However, when the bacteria start causing damage, the body begins to send signals. It’s important not to dismiss these as “just a sensitive stomach.”
Commonly reported H. pylori symptoms include:
The Burning Ache: A dull or burning pain in the abdomen, especially when the stomach is empty (between meals or in the middle of the night).
Persistent Bloating: Feeling excessively full even after eating a small amount of food.
Frequent Burping: Chronic belching that feels out of character for your usual digestion.
Nausea: A low-grade “queasiness” that may come and go throughout the day.
Loss of Appetite: A sudden lack of interest in food, often accompanied by unintentional weight loss.
If these symptoms progress to peptic ulcer disease, the signs become more acute. You might notice dark, tarry stools or vomit that looks like coffee grounds. If you experience these severe signs, it is vital to seek an immediate evaluation with a specialist like Dr. Samir Rahmani to prevent complications like perforation or internal bleeding.
From Gastritis to Peptic Ulcers: The Progression
To understand the impact of Helicobacter pylori, we have to look at the relationship between the bacteria and the stomach’s architecture.
What is Gastritis?
Gastritis is the inflammation, irritation, or erosion of the lining of the stomach. When H. pylori is the cause, it is known as chronic active gastritis. This isn’t a temporary irritation like you might get from eating spicy food; it’s a persistent immune response. The body tries to fight the bacteria, but because the bacteria are hidden in the mucus layer, the immune cells end up damaging the stomach’s own cells instead.
The Development of Stomach Ulcers
If the gastritis goes untreated, the protective lining wears thin. This allows stomach acid to eat away at the digestive tract’s tissue, creating an open sore. This is a stomach ulcer (or gastric ulcer). If it occurs in the first part of the small intestine, it is called a duodenal ulcer. Collectively, these are known as peptic ulcer disease.
While people used to believe that stress or spicy food caused ulcers, we now know that H. pylori is the culprit in the vast majority of cases. Stress might make the symptoms feel worse, but it doesn’t create the ulcer—the bacteria do.
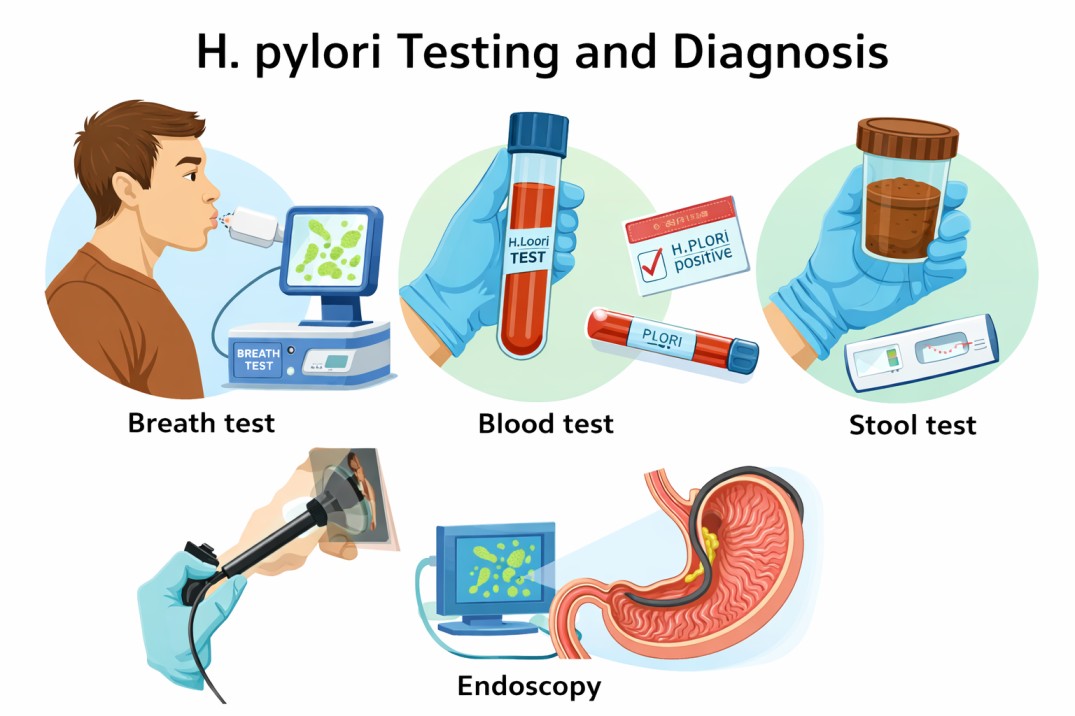
Testing and Diagnosis: Finding the Culprit
If you suspect a stomach infection, the next step is a definitive H. pylori test. Modern medicine has moved away from invasive procedures as the first line of defense, though they still have their place.
Dr. Samir Rahmani typically recommends one of the following diagnostic paths:
Urea Breath Test (UBT): This is often the “gold standard” for non-invasive testing. You swallow a liquid or capsule containing a tagged carbon atom. If H. pylori is present, it breaks down the substance and releases the carbon in your breath, which is then measured.
Stool Antigen Test: This looks for traces of the bacteria in a stool sample. It is highly accurate and commonly used to confirm if a H. pylori treatment has been successful.
Endoscopy: In cases where symptoms are severe or there is a risk of ulcers, a gastroenterologist may perform an endoscopy. A thin tube with a camera is passed into the stomach to look at the lining directly and take a tiny tissue sample (biopsy) for testing.
How Do You Get H. Pylori? A Deep Dive into Causes, Spread, and Risk Factors
H. Pylori Treatment: The Path to Eradication
Eradicating a helicobacter pylori infection requires a strategic and disciplined approach. Because the bacteria are quite resilient, a single antibiotic is rarely enough. Instead, doctors use “Combination Therapy.”
The Protocol
H. pylori treatment usually involves a 10 to 14-day course of medications:
Antibiotics: Usually two different types (such as Clarithromycin and Amoxicillin) to ensure the bacteria cannot develop resistance.
Proton Pump Inhibitors (PPIs): Drugs like Omeprazole or Esomeprazole that reduce stomach acid. Lowering the acid helps the antibiotics work more effectively and allows the stomach lining to heal.
Bismuth Subsalicylate: Sometimes added to the regimen (Quadruple Therapy) to help coat the ulcer and kill the bacteria.
It is absolutely crucial to finish the entire course of medication, even if you start feeling better after three days. Stopping early is a primary reason why stomach bacterial infections recur and become harder to treat later.
Diet and Lifestyle: Supporting Your Recovery
While medication kills the bacteria, your lifestyle choices dictate how quickly your stomach heals. Diet doesn’t “cure” H. pylori, but it certainly manages the gastritis symptoms and supports the mucosal lining.
What to Eat
Probiotics: Yogurt, kefir, and sauerkraut contain “good” bacteria that can help balance the gut microbiome during antibiotic treatment.
Fiber-rich foods: Whole grains, beans, and vegetables are generally well-tolerated and promote healthy digestion.
Flavonoids: Foods like broccoli, berries, and green tea may have properties that inhibit the growth of H. pylori.
What to Avoid
Irritants: Alcohol, smoking, and caffeine can exacerbate inflammation.
NSAIDs: Medications like ibuprofen or aspirin can further damage the stomach lining and should be avoided unless specifically cleared by your doctor.
Spicy and Acidic Foods: While they don’t cause the infection, they can trigger pain in an already inflamed stomach.
Why Professional Guidance Matters
Navigating a gastritis treatment or an ulcer recovery plan shouldn’t be a solo endeavor. Dr. Samir Rahmani emphasizes that every patient’s gut health is unique. Factors like age, medical history, and previous antibiotic use influence which treatment protocol will be most effective.
Furthermore, follow-up is essential. A common mistake is assuming the bacteria are gone because the pain stopped. Dr. Rahmani insists on a re-test (usually a breath or stool test) four weeks after treatment ends to ensure the H. pylori infection is completely eradicated.
Final Thoughts on Digestive Health
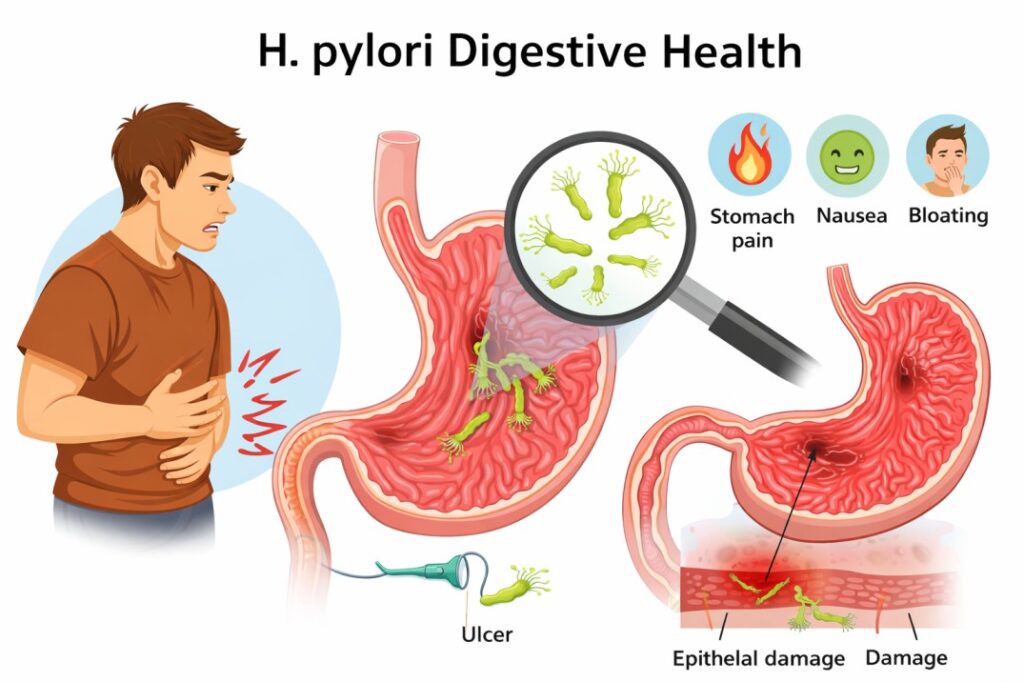
A diagnosis of H. pylori can feel overwhelming, but it is a manageable and treatable condition. The key is to move away from temporary fixes and toward a clinical solution that addresses the root cause of the inflammation. By understanding the nature of this stomach bacterial infection, recognizing the symptoms of gastritis, and committing to a professional treatment plan, you can protect your long-term digestive health.
If you are struggling with persistent stomach pain or suspect you may have an infection, seeking a consultation with an expert like Dr. Samir Rahmani is the most effective path forward. Your stomach works hard for you every day; it deserves the care and attention required to stay healthy.
Medical Disclaimer
This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified health provider with any questions you may have regarding a medical condition.
Medically reviewed by Dr. Samir Rahmani.
FAQs
Generally, no. While the immune system may keep it in check, the bacteria are specifically designed to survive the stomach environment indefinitely. Without medical intervention, the infection usually persists for life, potentially leading to chronic gastritis or ulcers.
Yes, it is considered contagious. It is primarily spread through saliva or fecal-oral routes. This is why it often runs in families; shared utensils, kissing, and close living quarters facilitate the spread.
Untreated infection can lead to persistent peptic ulcer disease, internal bleeding, and in rare cases, an increased risk of stomach cancer (gastric adenocarcinoma). Early detection is the best way to mitigate these risks.
It is generally discouraged. NSAIDs like ibuprofen can irritate the stomach lining and, when combined with an H. pylori infection, significantly increase the risk of developing a stomach ulcer.
Most patients begin to feel a reduction in stomach infection symptoms within a few days of starting treatment, as the PPIs reduce acid production. However, full healing of the stomach lining can take several weeks.
While some natural substances like Manuka honey or cranberry juice show anti-bacterial properties in laboratory settings, there is no scientific evidence that they can replace medical H. pylori treatment. They are best used as complementary support under a doctor’s guidance.
Sometimes, the antibiotics used to kill H. pylori can temporarily disrupt the balance of your gut microbiome, leading to “post-infectious” symptoms. Additionally, if the gastritis was severe, it may take longer for the tissue to fully settle.
Yes, the Urea Breath Test is highly accurate—typically over 95%. However, you must stop taking PPIs and antibiotics for at least two weeks before the test to avoid a “false negative” result.
While H. pylori is often associated with weight loss due to nausea and loss of appetite, some studies suggest that after successful treatment, patients may gain weight as their appetite returns and their digestion improves.
It can. The bacteria produce gases and enzymes that may contribute to halitosis (chronic bad breath). Many patients notice their breath improves significantly after successful H. pylori treatment.
Yes, many people are first infected during childhood. Symptoms in children may include abdominal pain, vomiting, or iron-deficiency anemia that doesn’t respond to supplements.
Not necessarily. Some ulcers are “silent” and don’t cause significant pain until they bleed or cause a blockage. This is why diagnostic testing is so important for those with persistent digestive issues.
You should undergo a follow-up H. pylori test (breath or stool) at least four weeks after finishing your medication. This is the only way to be certain the bacteria have been eliminated.
Re-infection is possible but relatively rare in adults once the initial infection is cleared. Practicing good hygiene and ensuring access to clean water are the best ways to prevent a recurrence.
While they can have overlapping symptoms like heartburn, they are different. GERD is caused by stomach acid flowing back into the esophagus, while H. pylori is a bacterial infection of the stomach lining itself. However, H. pylori can sometimes make GERD symptoms more complex.
MORE ARTICLES
Mounjaro and Your Organs: Thyroid, Kidney, Eye, and Liver Side...Read More
Mounjaro Side Effects by Dose: What to Expect at Every...Read More
Mounjaro Side Effects for Non-Diabetics: What Weight Loss Patients Need...Read More
Mounjaro Long-Term Side Effects: Cancer Risk, Safety Concerns, and What...Read More