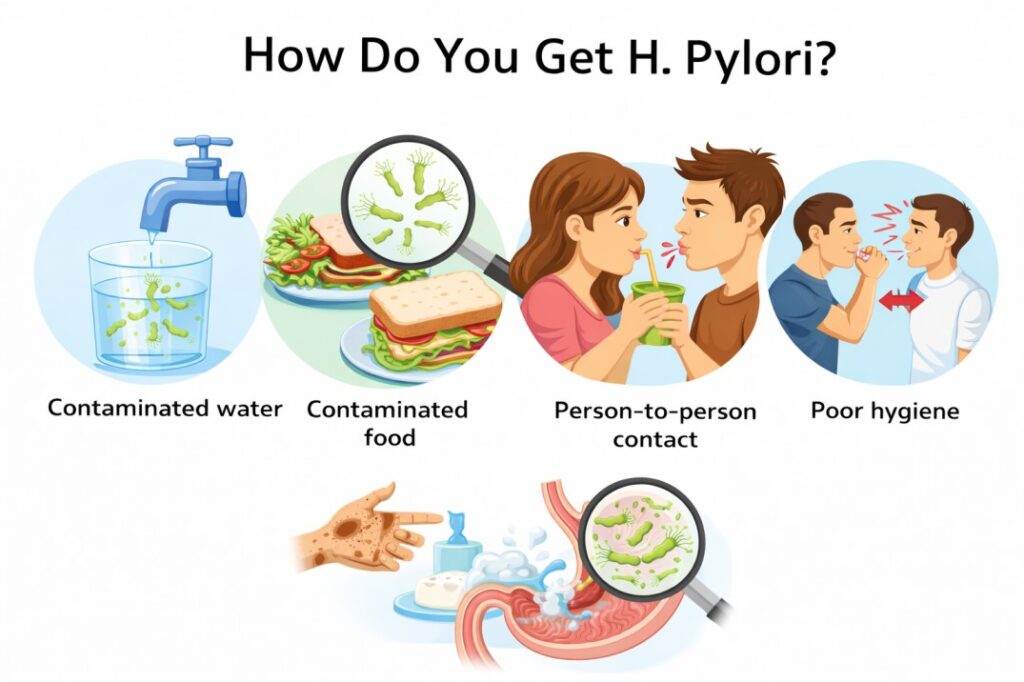
How Do You Get H. Pylori? A Deep Dive into Causes, Spread, and Risk Factors
By Dr. Samir Rahmani, FRCS (England), UK-Trained Laparoscopic, Bariatric & GI Surgeon, Dubai | Medically Reviewed: March 2026

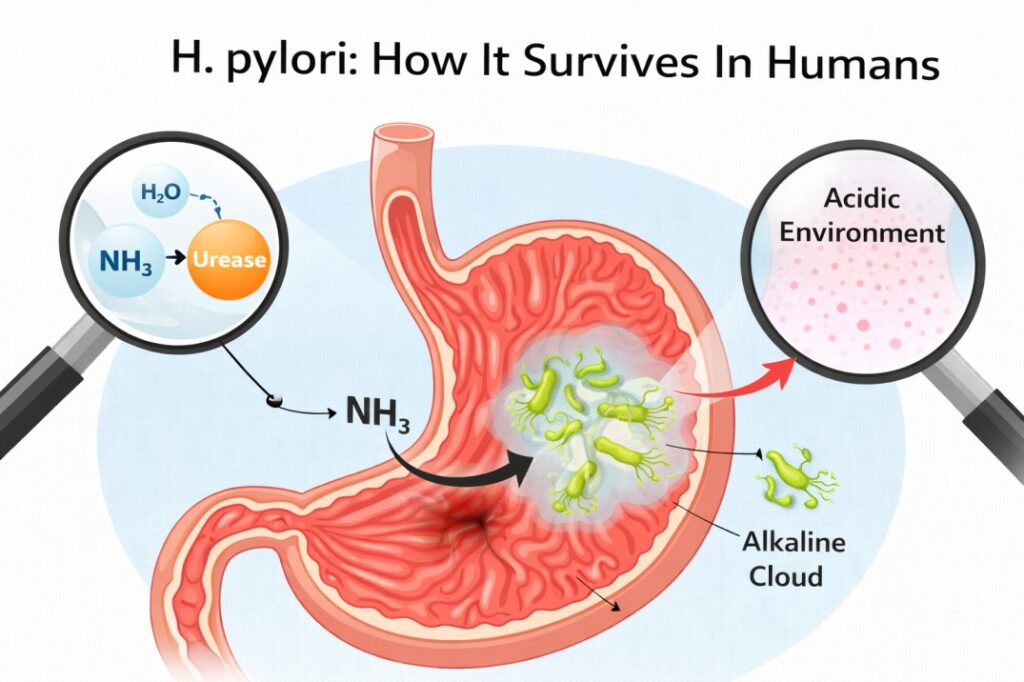
The human stomach is a remarkably hostile environment. It is a churning vat of hydrochloric acid designed to dissolve food and annihilate most bacteria on contact. Yet, Helicobacter pylori—or h pylori—doesn’t just survive there; it thrives. If you have recently discovered you have this infection, or if a family member has, the first question that almost always arises is: “How did this happen?” Understanding how do you get h pylori isn’t just about satisfying a medical curiosity. It’s about understanding the invisible pathways through which this resilient bacterium moves between people and environments. It’s a bit of a detective story, really. One that takes us through the nuances of h pylori transmission and into the quiet ways our daily habits might invite an uninvited guest into our digestive system.
Dr. Samir Rahmani often tells his patients that while the diagnosis can feel a bit jarring, it is incredibly common—nearly half the global population carries it. But where does h pylori come from, and why do some people get sick while others never know they have it? Let’s peel back the layers of these causes of h pylori infection.
The Root of the Problem: Where Does H. Pylori Come From?
To understand what causes h pylori infection, we have to look at the bacteria itself. It’s a spiral-shaped organism with tail-like flagella that allow it to “screw” itself into the protective mucus lining of the stomach. This isn’t a bacteria that usually drops out of the sky or appears from nowhere.
Historically, h pylori transmission is deeply tied to the environment. In many parts of the world, particularly where clean water and modern sewage systems are still developing, the bacteria are ubiquitous. It is often found in contaminated water sources or soil. However, even in highly developed urban environments, the infection persists. This suggests that while environmental factors are a starting point, the primary way how do people get h pylori is through more intimate, human-to-human contact.
Is H. Pylori Contagious?
This is perhaps the most frequent question in clinical consultations. The short answer is: Yes, absolutely. However, it isn’t “contagious” in the way a cold or the flu is. You aren’t going to catch it just by standing in the same room as someone. How contagious is h pylori depends heavily on hygiene and close contact. It is generally passed through direct contact with saliva, vomit, or fecal matter.
The Pathways of Transmission: How Is H. Pylori Spread?
The medical community generally categorizes how is h pylori spread into two main routes: fecal-oral and oral-oral.
1. The Fecal-Oral Route
This sounds unpleasant, but it is a primary driver of infection globally. If someone carries the bacteria and doesn’t wash their hands thoroughly after using the bathroom, they can transfer the bacteria to surfaces, food, or other people. This is especially prevalent in households with young children who are still learning hygiene habits.
2. The Oral-Oral Route
This involves the transfer of bacteria through saliva. This brings us to a very personal question many patients hesitate to ask: can you get h pylori from kissing? Because the bacteria can reside in the dental plaque and saliva of an infected individual, deep kissing can potentially transfer the organism. It’s one of the reasons why, when Dr. Samir Rahmani treats a patient for a recurring infection, he sometimes suggests that their partner also get screened.
3. Contaminated Food and Water
If you’ve ever wondered how do you contract h pylori while traveling, the answer often lies in the kitchen. If food is washed with contaminated water or handled by someone with the infection who hasn’t practiced proper hand hygiene, the bacteria can easily find a new host.
Why Me? Risk Factors and Vulnerability
Knowing how do you get h pylori is only half the battle; the other half is understanding why the bacteria decides to stay.
Living Conditions: Living in crowded housing where many people share small spaces increases the likelihood of spread.
Water Supply: Lack of a reliable source of clean, treated water is perhaps the single biggest risk factor for what causes h pylori infection on a global scale.
Childhood Environment: Most people actually contract h pylori during childhood. Their immune systems are still developing, and children are naturally less focused on hand hygiene.
Family Members: If someone in your immediate home has the infection, your risk increases exponentially due to shared bathrooms, kitchens, and close physical affection.
H. Pylori Symptoms: Early Warning Signs You Should Never Ignore
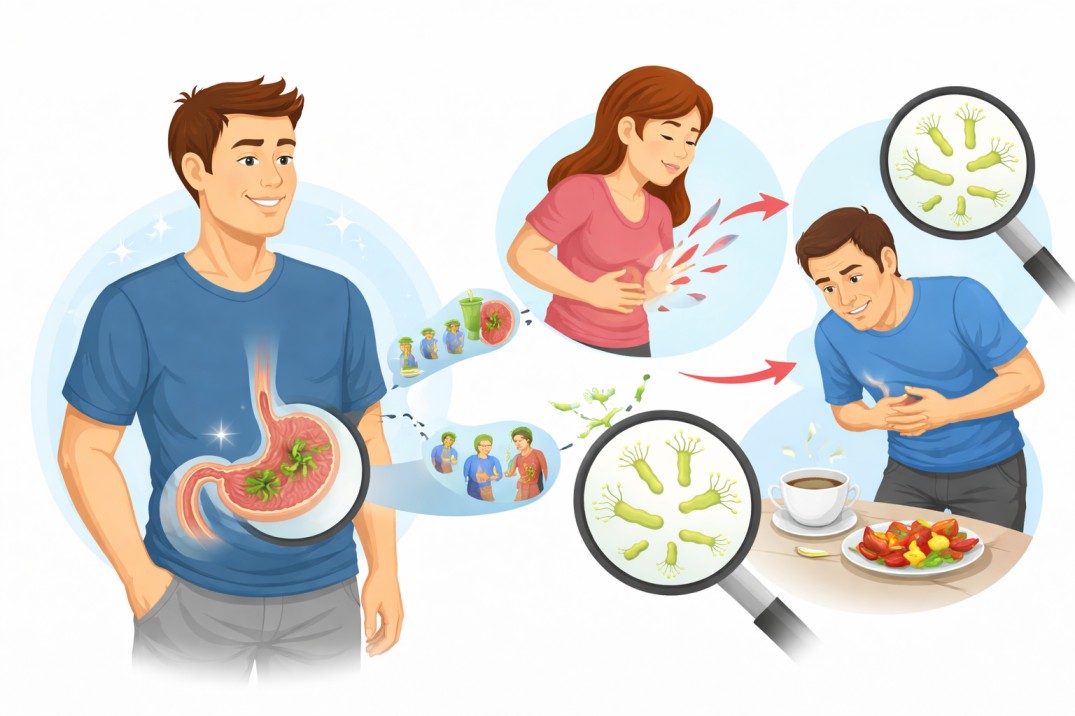
The Mystery of the Asymptomatic Carrier
A fascinating, albeit frustrating, aspect of this infection is that many people carry the bacteria for their entire lives without ever knowing it. They have no pain, no ulcers, and no symptoms. Why? It likely comes down to a combination of the specific strain of the bacteria and the host’s genetic immune response. However, even if you are asymptomatic, you can still be a source of h pylori transmission to others who might be more vulnerable to developing ulcers or gastritis.
Diagnosis: How Do We Know It’s There?
If you suspect you’ve been exposed—perhaps because a partner was diagnosed or you’re experiencing that telltale gnawing stomach pain—the next step is testing. Dr. Samir Rahmani utilizes several highly accurate methods or tests to check for the bacteria:
The Urea Breath Test: You swallow a special liquid, and we measure the carbon dioxide in your breath. It’s simple, non-invasive, and incredibly accurate.
Stool Antigen Test: This checks for the presence of the bacteria directly in a stool sample.
Endoscopy: In more complex cases, a small camera is used to look at the stomach lining and take a biopsy.
Preventing the Spread: Breaking the Cycle
Since we know how is h pylori spread, we can take very specific steps to prevent it. It isn’t about living in a sterile bubble; it’s about basic, consistent hygiene.
The 20-Second Rule: Wash your hands with soap and water after using the restroom and before preparing or eating food. This is the single most effective way to stop the fecal-oral route.
Clean Water: If you are in an area where water quality is questionable, stick to boiled or bottled water, even for brushing your teeth.
Food Safety: Ensure food is cooked thoroughly and washed with clean water.
Screening the Household: If one person is diagnosed and treated but the rest of the family isn’t tested, the bacteria can simply “ping-pong” back and forth between family members.
Understanding the Long-Term Impact
If the causes of h pylori infection are left unaddressed, the bacteria continues to erode the stomach’s protective lining. This can lead to:
Gastritis: Persistent inflammation.
Peptic Ulcers: Open sores in the stomach or duodenum.
Stomach Cancer: In a small percentage of cases, chronic inflammation can lead to malignancy.
This is why Dr. Samir Rahmani emphasizes that treatment isn’t just about stopping the current stomach ache—it’s about cancer prevention and long-term gastrointestinal health.
The Path to Eradication with Dr. Samir Rahmani
Treatment is a collaborative effort. It typically involves a combination of antibiotics and acid-suppressing medications. It’s not a “one-pill” fix. It requires discipline—finishing every single dose even if you feel better on day three.
Dr. Rahmani’s approach focuses on the whole patient. It isn’t just about killing the bacteria; it’s about healing the stomach lining and educating the patient on how to prevent re-infection. This includes discussing h pylori transmission risks within the family and ensuring that the recovery process is monitored with follow-up testing.
Why Professional Guidance is Non-Negotiable
You might see “natural” remedies online—clove oil, manuka honey, or green tea. While these may have mild antibacterial properties, they are not a substitute for medical treatment. Helicobacter pylori is an expert at survival; it will not be intimidated by honey. Relying on unproven methods only gives the bacteria more time to cause damage.
Living Post-H. Pylori: What Changes?
Once the bacteria is gone, many patients feel like a cloud has lifted. The constant bloating, the “hunger pains” that aren’t hunger, and the fatigue often vanish. However, the stomach needs time to find its rhythm again.
Probiotics: After a heavy course of antibiotics, replenishing the “good” bacteria is essential.
Dietary Adjustment: Avoiding irritants like excessive caffeine or spicy foods for a few weeks gives the stomach lining a chance to fully regenerate.
Ongoing Vigilance: Continue those good hygiene habits. Just because you’ve had it once doesn’t mean you are immune for life.
A Note of Perspective
When you’re dealing with a diagnosis, it’s easy to over-analyze every interaction. “Did I get this from that restaurant? Did I get this from my spouse?” The truth is, how do you get h pylori is often a question with a complex answer that goes back years.
What matters most is the present. Modern medicine has made the diagnosis and eradication of this bacteria straightforward. Under the care of a specialist like Dr. Samir Rahmani, you aren’t just getting a prescription; you’re getting a roadmap back to a healthy gut.
Take a deep breath. Practice your hygiene. Follow your treatment plan. Your stomach is a resilient organ, and with the right help, it can return to its intended job: nourishing you without pain.
Next Steps for Your Health:
If you suspect you have been exposed or are experiencing recurring digestive issues, a consultation is the first step toward clarity. Dr. Samir Rahmani offers specialized diagnostic testing and personalized treatment plans to ensure your digestive system is protected for the long term.

About the author
Dr. Samir Rahmani
FRCS (England)
CCT General Surgery (UK)
MD — University of Leeds
MSc Surgery — University of Hull
27+ years experience
5,000+ procedures
Dr. Samir Rahmani is a UK-trained consultant surgeon with 27+ years of experience in bariatric, gastrointestinal, and metabolic health management. He completed advanced surgical training in the UK and previously served at Aneurin Bevan University Health Board (NHS Wales).
He holds an MD in Surgery from the University of Leeds and is JAG-accredited in GI endoscopy. Currently practicing in the UAE, he provides evidence-based guidance on weight loss treatments, including medications like Mounjaro (tirzepatide), with a focus on monitoring organ-related side effects involving the thyroid, kidneys, eyes, and liver to ensure safe and personalised care.
FAQs
The bacteria are quite fragile once they are outside the human body or a water source. They don’t typically survive for long on dry surfaces like countertops, but they can persist on moist surfaces or in improperly cleaned kitchen sponges.
It largely correlates with socioeconomic factors. Access to treated water and less crowded living conditions significantly reduce what causes h pylori infection spread.
Yes, but it’s usually one of two things: either the first treatment didn’t fully kill all the bacteria (resistance), or the person was re-infected by a household member who was never treated.
Yes. As we discussed regarding h pylori contagious through air, simply sleeping near someone is not a risk. The risk lies in shared saliva or poor hand hygiene.
Yes, if the vegetables were grown in soil contaminated with the bacteria or washed with contaminated water. This is why thorough washing is always recommended.
Currently, there is no commercially available vaccine. Prevention relies entirely on hygiene and early treatment.
No. This is a common myth. Stress doesn’t “create” bacteria. However, stress can make the symptoms of an existing infection much worse by increasing stomach acid.
Soap and water are the most effective. Alcohol-based sanitizers can help, but they are not a replacement for the physical act of washing away bacteria.
It’s a common concern at family dinners or among friends. Theoretically, yes, because the bacteria can be present in saliva. If an infected person has a high bacterial load and you drink immediately after them, there is a risk. While not as common as other forms of spread, it is a reason why Dr. Samir Rahmani recommends individual glasses and cutlery if a household member is currently undergoing treatment.
This is a point of confusion for many. Unlike respiratory viruses (like COVID-19 or the common cold), h pylori contagious through air transmission is not a recognized pathway. You cannot catch it through sneezing, coughing, or simply breathing the same air as an infected person. It requires a more direct “fluid-to-fluid” or “fecal-to-food” connection.
This is critical for household management. You remain contagious as long as the bacteria are active in your system. Once you begin the triple or quadruple antibiotic therapy prescribed by a specialist like Dr. Samir Rahmani, the bacterial load drops significantly. However, you aren’t considered “non-contagious” until a follow-up test (usually 4 weeks after treatment) confirms the infection is completely eradicated.
It’s important not to feel “guilty” or “unclean” if you have this infection. Because it is so often contracted in childhood, you may have been carrying it for decades before it ever caused a symptom. It could have come from a shared toy in a playground thirty years ago or a glass of water on a childhood vacation. The focus should be on treatment now, not on pinpointing a source from the distant past.
While there is some evidence that certain strains of Helicobacter can exist in cats or dogs, the risk of getting the standard human h pylori from a pet is considered extremely low. Most infections are human-to-human.
If the pool is properly chlorinated, the bacteria shouldn’t survive. However, in untreated lakes or stagnant water, the risk of h pylori transmission through accidental swallowing is higher.
Medical Disclaimer
This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified health provider with any questions you may have regarding a medical condition.
Medically reviewed by Dr. Samir Rahmani.